
Are Paediatrics Being Left Out of the Equation?
Helping Save Paediatric Lives
Olivia Quigley was six years old when she suffered sudden cardiac arrest (SCA). She was in first grade, doing warm-ups in gym class, when she suddenly collapsed.
She was fortunate that her school had rehearsed an immediate medical emergency response plan. After two teachers performed six minutes of cardiopulmonary resuscitation (CPR), paramedics arrived with a defibrillator that revived Olivia. She survived. Recounting the experience, her father says, “Cardiac arrest isn’t rare – survival is.” 1
Each year in the United States, over 7,000 children experience an out-of-hospital cardiac arrest (OHCA).2 Their chances of survival are largely dependent on whether bystanders and practitioners act with the same confidence and skill set with which they would treat an adult.3
Only 9% of children survive, and many have poor neurological outcomes.4
Olivia’s story shows the best possible outcome for a paediatric victim of SCA. Witnesses saw her collapse, teachers began bystander CPR right away, and EMS arrived within minutes to take over. Her survival is a testament to how preparation can make the difference between life and death. But, sadly, hands-on practice for paediatric patients can be overlooked. People don’t like to imagine doing CPR on a child.
In this article, we share an overview of the challenges presented in a paediatric SCA and discuss how increasing the frequency and quality of hands-on practice for paediatric resuscitation can help.
A Rundown of Paediatric Resuscitation Roadblocks
- Misperceptions can cause a roadblock to proper care. When one says “sudden cardiac arrest,” most people don’t envision a child. More than likely, they envision an elderly male patient with existing health concerns. Though that would reflect the average victim of SCA, it would not be an accurate representation of the true scope of victims. SCA can claim anyone – of any age, male or female, regardless if they have an existing heart condition.5
- Training for adult patients doesn’t prepare you for a paediatric patient. It’s self-evident that children are not like adults – anatomically, physiologically, or in their daily habits. So it’s not surprising that, in contrast to adults, coronary artery disease is rarely the cause of a paediatric SCA. Rather, paediatric arrest is generally caused by two conditions. One is progressive tissue hypoxia as the result of respiratory failure and/or shock.6 The other is a congenital heart condition that did not present symptoms until the event.7
- The unpredictability of sudden cardiac arrest leaves witnesses paralysed by unfamiliarity, surprise, and panic – and can hinder their willingness and ability to provide quality compressions and ventilations. 88% of paediatric OHCAs occur in non-public places.8 For those that are witnessed, many occur among young athletes. 1 in 70 high schools per year report a paediatric arrest.9 In all of these cases, witnessed or unwitnessed, providers are often ill prepared to act.
EMS and Healthcare Providers
Training for the unexpected is one of the many benefits offered through simulation. This can be particularly true for healthcare professionals who are more likely to treat adult patients and are now faced with a paediatric patient in SCA. Treating paediatric patients can often provoke a sense of anxiety and discomfort among EMS personnel.14 The EMS for Children Survey (April 2020) found that 43.6% of EMS agencies see, on average, fewer than one paediatric patient per month. 15 This indicates that there is certainly a lack of real-life paediatric practice.
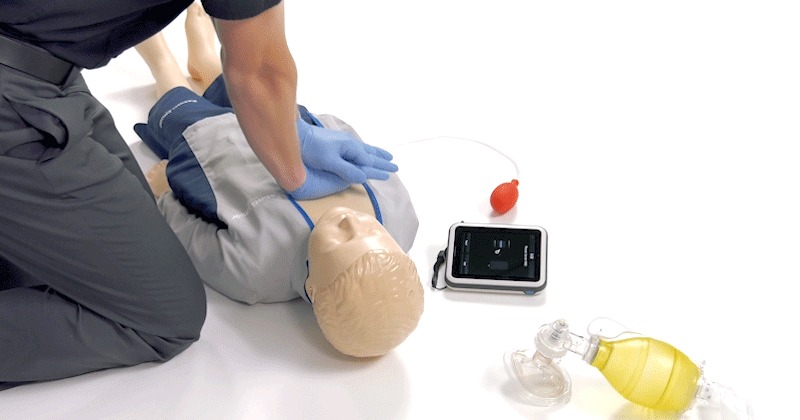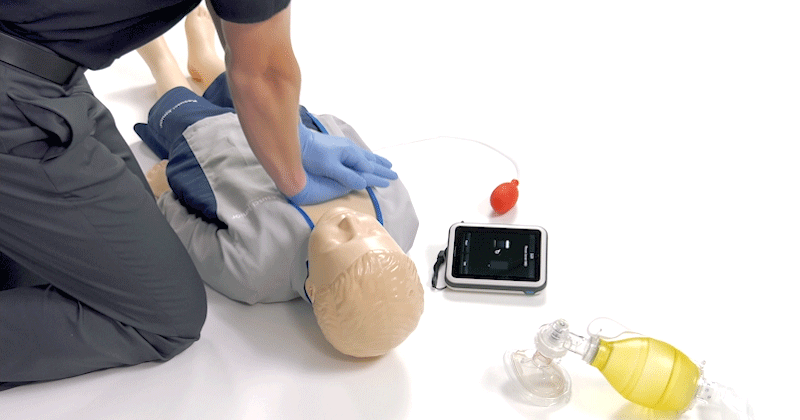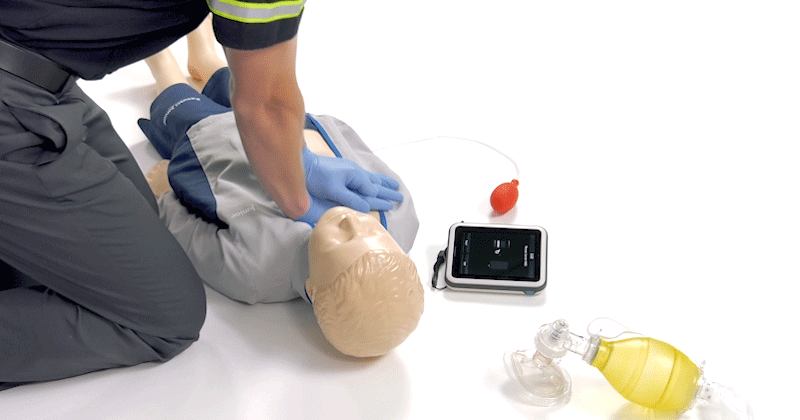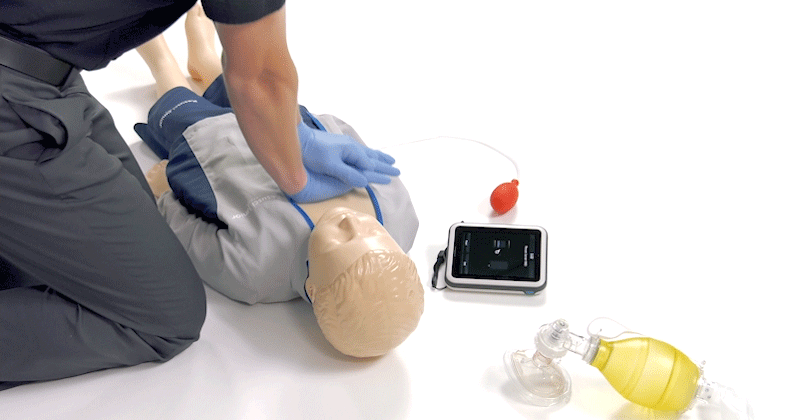 EMS professionals training for paediatric QCPR.
EMS professionals training for paediatric QCPR.
Over the past 30 years, pre-hospital survival rates have remained the same.15 This is in comparison to rates within hospitals, which have continuously increased.16
Why is this? According to Dr. Peter Antevy, many EMTs and paramedics have a tendency to automatically transport paediatric patients, as opposed to remaining to treat them on site as they would with adult patients. 17 When these first, critical minutes are used to transport patients, the chances of survival decrease. 18 This is precisely why training for paediatric victims is so important – developing the confidence and skills to stay put makes all the difference.
It’s important to note that, even though paediatric in-hospital survival rates are improving, survival is still the exception to the rule. According to the American Heart Association (AHA), there is only a 36% survival-to-discharge rate for paediatric in-hospital cardiac arrests (IHCA).19 The majority of children do not recover, even with immediate attention from healthcare professionals.
Research shows that only 10% of professionals achieve the necessary chest compression fraction, chest compression depth, and chest compression rate in a paediatric resuscitation.20 What all of this points to is the need for additional training – more specifically, training with a focus on high-quality CPR.
Quality CPR for paediatrics is no longer a guessing game. With training manikins that provide immediate feedback and corrective guidance, professionals can feel confident that they are applying life-saving techniques.
Quality Bystander Performance is Critical
Of the arrests that are witnessed, bystander CPR is only performed 35% of the time.10 Experts suggest that one way to improve paediatric survival rates is to build bystander confidence to take action.
One study found that a one-hour crisis resource management training improved the trainees’ response time in the initial steps in a paediatric resuscitation.11 And, another study found that self-efficacy increased and anticipated anxiety about CPR decreased one month after parents received CPR training.12 This research highlights the impact that quality CPR training can make within a community. Reducing the fear factor means increasing survival.
In order to effectively train community members in CPR and ensure that they will leave the classroom confident in their ability save a life, it helps to use more engaging learning methods. It’s been shown that learners achieve the greatest competency through interactive activities. Incorporating measurement, assessment, and feedback into paediatric CPR training can better prepare them for optimal performance, and can help you rest assured that you’ve just taught a class of future lifesavers.
To increase SCA survival rates for children, training needs to be geared toward the people who are most likely to be with them – parents, teachers, coaches, and even children as young as 9-years-old.13 Engaging courses that provide the paediatric practice that these learners need are one way to make the training stick.
A Low-Frequency, High-Acuity Void
Paediatric cardiac arrest is unsettling and challenging to treat. Children are less likely than adults to experience cardiac arrest, but that shouldn’t create a void for paediatrics in CPR training. Instead, training for these low-frequency, high-acuity events should be made equally as important.
By incorporating a paediatric manikin into your existing training curriculum, bystanders and healthcare professionals alike can improve their paediatric resuscitation skills. Laerdal Medical offers a range of paediatric CPR skills manikins that incorporate Quality CPR feedback and which will allow your learners to train to the highest CPR standards possible.
References
- Donaldson James, S. (2013). 6-year-old survives cardiac arrest because school had plan. ABC News. Retrieved from https://abcnews.go.com/Health/sudden-cardiac-arrest-kills-healthy-year/story?id=18381107
- Fuchs, S.M. (2018). Advocating for life support training of children, parents, caregivers, school personnel, and the public. The American Academy of Pediatrics. Retrieved from http://pediatrics.aappublications.org/content/early/2018/05/21/peds.2018-0705
- NYeHealth. (2016). Resuscitating the child: Disrupting the status quo to save our future at #DHC16. YouTube. Retrieved from www.youtube.com/watch?v=gjo_znxc2gw
- Fuchs, S.M. (2018). See reference #2.
- Sudden Cardiac Arrest Foundation. (2018). Sudden cardiac arrest: A healthcare crisis. Retrieved from http://www.sca-aware.org/about-sca
- Torrey, S.B. (2017). Pediatric basic life support for health care providers. UpToDate. Retrieved from https://www.uptodate.com/contents/pediatric-basic-life-support-for-health-care-providers
- Khan, B.V. (2018). Sudden cardiac arrest in kids: What and why? Sudden Cardiac Arrest Foundation. Retrieved from http://www.sca-aware.org/schools/sudden-cardiac-arrest-in-kids-what-and-why
- Fuchs, S.M. (2018). See reference #2.
- Ibid.
- Ibid.
- Blackwood, J., Duff, J.P., Nettel-Aguirre, A., Djogovic, D., & Joynt, C. (2014). Does teaching crisis resource management skills improve resuscitation performance in pediatric residents? Pediatric Critical Care Medicine. DOI: 10.1097/PCC.0000000000000100.
- Schlessel, J.S., Rappa, H.A., Lesser, M., Pogge, D., Ennis, R. & Mandel, L. (1995). CPR knowledge, self-efficacy, and anticipated anxiety as functions of infant/child CPR training. Annals of Emergency Medicine. Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/7741338
- CPR Consultants. (2017). What age should children learn cpr? Retrieved from https://www.cprconsultants.com/what-age-should-children-learn-cpr/
- Hewes, Hilary A., et al. "Ready for children: assessing pediatric care coordination and psychomotor skills evaluation in the prehospital setting." Prehospital Emergency Care 23.4 (2019): 510-518.
- National Emergency Medical Services for Children Data Analysis Center, “EMS for Children Survey,” April 2020
- Standford Medicine X. (2017). Peter antevy, MD: Redesigning the emergency medical response. YouTube. Retrieved from https://www.youtube.com/watch?v=er4PFGG67TM
- Ibid
- Ibid
- Ibid
- American Heart Association. (2018). Part 11: Pediatric basic life support and cardiopulmonary resuscitation quality. American Heart Association. Retrieved from https://eccguidelines.heart.org/index.php/circulation/cpr-ecc-guidelines-2/part-11-pediatric-basic-life-support-and-cardiopulmonary-resuscitation-quality/
- Niles, D., Duval-Arnould, J., Skellett, S., Knight, L., Su, F., Raymond, T., et al. (2018). Characterization of pediatric in-hospital cardiopulmonary resuscitation quality metrics across an international resuscitation collaborative. Pediatric Critical Care Medicine. DOI: 10.1097/PCC.0000000000001520
Learn More


